What Is Data Provenance? Meaning, Uses, And Vs. Lineage


What Is Data Provenance? Meaning, Uses, And Vs. Lineage
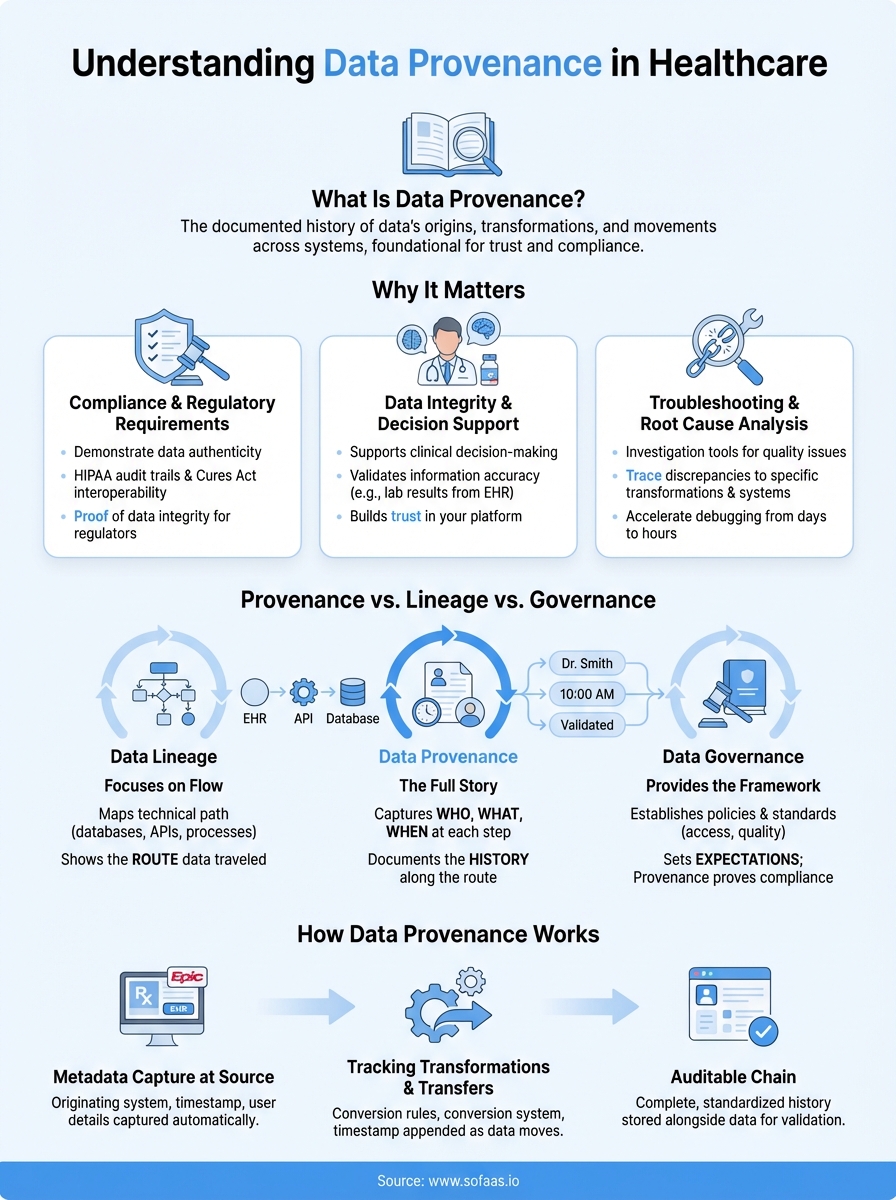
When patient data moves between systems, one question becomes critical: where did this data actually come from? What is data provenance answers exactly that, it's the documented history of data's origins, transformations, and movements across systems. For healthcare organizations integrating with EHRs, understanding provenance isn't optional; it's foundational to compliance and patient safety.
Data provenance tells you who created a record, when it was modified, and every system it passed through. This matters because healthcare applications must demonstrate that the information they display or act upon is accurate and trustworthy. At SoFaaS, we've built our SMART on FHIR integration platform with data integrity at its core, enabling healthcare innovators to maintain clear provenance as patient data flows between their applications and EHR systems.
This article breaks down data provenance, what it means and why it's essential, and clarifies how it differs from data lineage and data governance. Whether you're building a new healthcare application or scaling existing EHR integrations, understanding these distinctions will help you design systems that stakeholders and regulators can trust.
Why data provenance matters
Understanding what is data provenance becomes essential when you consider that healthcare decisions rely on data accuracy. Every patient record that flows through your application carries legal and clinical implications, and you need to prove that the information you're presenting came from legitimate sources. Without clear provenance, you expose your organization to compliance violations, liability risks, and potentially harmful clinical decisions based on unverified information.
Compliance and regulatory requirements
Healthcare regulations demand you demonstrate data authenticity at every stage. HIPAA requires you to maintain audit trails showing who accessed patient information and when modifications occurred. The 21st Century Cures Act pushes data interoperability forward, but that means you must prove that the data you share or receive maintains its integrity throughout transmission. If auditors or regulators question your data sources, provenance documentation provides the evidence you need to validate your compliance posture.
Provenance serves as your organization's proof that patient data remained accurate and unaltered throughout its journey across systems.
Data integrity and decision support
You build healthcare applications to support clinical decision-making, which means clinicians must trust the information you provide. Provenance metadata tells users whether lab results came directly from an EHR or passed through intermediate systems where transformations might have occurred. When a physician reviews patient allergies in your application, provenance confirms these records originated from verified sources rather than outdated caches or unvalidated imports. This transparency builds confidence in your platform and protects patients from decisions based on questionable data.
Troubleshooting and root cause analysis
Data quality issues will arise in healthcare integrations, and provenance gives you the investigation tools you need. When you spot discrepancies between your application and the source EHR, provenance records show exactly where data transformations happened and which systems touched the information. You can trace a corrupted record back to the specific API call, timestamp, and system version that introduced the error. This capability accelerates debugging from days to hours and helps you implement targeted fixes rather than broad system changes that might introduce new problems.
Data provenance vs data lineage and governance
Understanding what is data provenance requires distinguishing it from related concepts that healthcare teams often confuse. While data lineage, governance, and provenance all support data quality and compliance, each serves distinct purposes in your integration architecture. Clarifying these differences helps you implement the right tracking mechanisms and avoid building redundant systems that create unnecessary overhead.

Data lineage focuses on flow
Data lineage maps the technical path data follows through your systems, showing you which databases, APIs, and transformation processes touched each record. You use lineage to understand system dependencies and trace data flows across your architecture. Provenance goes deeper by capturing who, what, and when at each step, not just the route data traveled. When a lab result moves from an Epic EHR through your application's transformation layer to your analytics database, lineage shows the three-step path, while provenance documents the originating physician, timestamp of each transformation, and validation rules applied at every stage.
Lineage tells you the route your data takes; provenance tells you the story of what happened to it along that route.
Governance provides the framework
Data governance establishes the policies and standards you enforce across your organization, defining who can access patient records and what quality thresholds you require. Provenance serves as the enforcement mechanism that proves you're following those governance rules. Your governance framework might mandate that medication data comes only from certified EHR sources, while provenance metadata provides the auditable evidence that each medication record actually originated from an approved system. You need governance to set expectations and provenance to demonstrate compliance with those expectations.
How data provenance works
Data provenance operates through metadata capture at every point where data gets created, modified, or transferred. When your application pulls a patient record from an Epic EHR through the SoFaaS platform, the system automatically logs the originating system identifier, timestamp, API endpoint called, and authentication credentials used. This metadata travels alongside the actual patient data, creating an auditable chain that you can reference later when questions arise about data authenticity or compliance.
Metadata capture at source
The process starts when data enters your ecosystem. Your integration layer captures source system details, including the EHR vendor, facility identifier, and user who initiated the data request. This initial metadata forms the foundation of your provenance chain. If you're pulling medication lists from Cerner, the system records not just the medications but also which Cerner instance provided them, which SMART on FHIR scope authorized the access, and what version of the FHIR specification formatted the response.
Capturing metadata at the point of origin ensures you maintain an unbroken chain of custody throughout the data's lifecycle.
Tracking transformations and transfers
Every time your application transforms or moves data, you append transformation metadata to the provenance record. When you normalize medication codes from proprietary formats to standard terminologies, you log the conversion rules applied, the timestamp of transformation, and the system component that performed the work. This creates a complete history showing not just what changed but also why and when those changes occurred, which proves essential when regulators ask you to demonstrate data integrity across your integration pipeline.
![]()
How to document data provenance
Documenting data provenance requires you to establish systematic processes that capture metadata automatically rather than relying on manual tracking. You need standardized formats for recording source information, transformation details, and access patterns that create consistent audit trails across your entire integration environment. The key lies in building provenance capture directly into your data pipelines so documentation happens as a natural byproduct of your normal operations rather than as an afterthought.
Establishing metadata standards
You must define which provenance attributes matter for your healthcare application before you start capturing anything. Standard elements include source system identifiers, timestamps in ISO 8601 format, user authentication details, and version numbers for both data and transformation logic. Your metadata schema should align with FHIR Provenance resources when working with EHR integrations, which provides a standardized structure that other healthcare systems can interpret. This consistency ensures that when you share data with partners or demonstrate compliance to auditors, your provenance records follow recognized industry patterns that stakeholders understand.
Standardized metadata schemas prevent you from collecting useless information while ensuring you capture everything regulators and clinical users need.
Implementing automated capture
Building provenance into your integration middleware eliminates the human error that comes with manual documentation. You configure your SMART on FHIR integration layer to automatically append provenance metadata each time it retrieves patient data from an EHR or processes a transformation. Modern integration platforms like SoFaaS handle this capture natively, logging source attribution and transformation details without requiring custom code. Your application receives both the clinical data and its complete provenance history through standardized API responses, which you can store alongside the data itself or in separate audit tables depending on your architecture needs.
Data provenance use cases and examples
Understanding what is data provenance becomes concrete when you examine real scenarios where provenance tracking prevents errors and enables compliance. Healthcare organizations use provenance to validate clinical decision support, demonstrate regulatory compliance, and enable secure research collaborations. These examples show how provenance metadata protects patients while supporting the data sharing that modern healthcare requires.
Clinical decision support systems
Your application displays medication alerts based on patient allergy records, but how do you prove those allergy records came from verified sources rather than outdated manual entries? Provenance metadata shows that the allergy list originated from the patient's primary EHR, was last updated by their physician three days ago, and passed through your SMART on FHIR integration without modifications. When a clinician questions an alert, you can trace the exact source and timestamp of the triggering data, which builds trust in your system's recommendations and protects against liability from incorrect alerts.
Provenance transforms clinical alerts from black box warnings into transparent recommendations backed by verifiable data sources.
Regulatory audits and compliance verification
Auditors demand proof that your application maintains HIPAA compliance throughout data exchanges. You present provenance records showing every instance where patient data entered your system, which users accessed specific records, and when you transmitted information to external parties. The audit trail demonstrates that your authentication mechanisms functioned correctly and that data remained encrypted during transmission, providing the documented evidence regulators require without manual report generation.
Research data sharing
Healthcare researchers need de-identified patient data from multiple institutions, but participating organizations must verify that data maintains integrity throughout aggregation. Provenance records prove which hospital systems contributed each dataset, what de-identification rules were applied, and which transformation processes normalized the data for analysis, enabling collaborative research while maintaining accountability across institutional boundaries.
Final takeaways
Understanding what is data provenance gives you the foundation to build healthcare applications that stakeholders trust. You now know that provenance documents the complete history of your data, including its origins, transformations, and movements across systems. This differs from lineage, which tracks technical paths, and governance, which establishes policies, because provenance provides the auditable evidence that proves your compliance and protects patient safety.
Healthcare integrations demand accurate data tracking at every stage. Your application must capture metadata automatically, maintain standardized formats, and preserve provenance chains throughout data exchanges. These practices enable you to demonstrate regulatory compliance, support clinical decisions with verifiable information, and troubleshoot issues rapidly when problems arise.
Building these capabilities requires robust infrastructure that handles provenance natively. Launch your SMART on FHIR integration with SoFaaS and get built-in provenance tracking that maintains audit trails automatically, letting you focus on building innovative healthcare solutions rather than compliance infrastructure.
The Future of Patient Logistics
Exploring the future of all things related to patient logistics, technology and how AI is going to re-shape the way we deliver care.